Why do I have my stoma?
I had my stoma surgery in June 2018, after having been on a liquid diet for just over a year (I was drinking Ensure Nutritional Supplement drinks – the Juce Plus ones were lactose free so I had them). I had around 6 of these a day. I’d been having stomach problems since the age of 10, becoming more serious when I was 14. I eventually had various tests, including a diagnosis of hypermobile Ehlers Danlos Syndrome, that determined what was wrong with my digestive system. I had colonic inertia, a rectocele, a rectal intussusception and a very slight anal prolapse due to my connective tissue being more ‘stretchy’ and so my colon and rectum had less muscular support – you need that in order for peristalsis to work efficiently (where the muscular wall of the intestines contract to ‘move’ waste along).
This made me severely constipated – hence why I ended up being on the Ensure drinks. I also had to have lots of laxatives (Movicol, Docusate, Prucalopride and Mintec Peppermint Capsules). After speaking to various hospitals/surgeons, I finally found someone (at St Mark’s Hospital, Harrow, London – specialist bowel hospital) who agreed that I needed help and that one of the only ways was to have an ileostomy – which is when a bit of my small intestine sticks out my stomach and a bag goes over it to ‘collect’ the waste – this would bypass my problematic colon and rectum. Today, I can eat whatever I want and can finally live life more to the full! Medication wise, I take 2 Sando K potassium dissolvable tablets (as I need more potassium to stay hyrated due to my colon being ‘out of action’).
How did I get my Ehlers Danlos Syndrome (EDS) diagnosis?
I was extremely lucky to get a diagnosis fairly quickly – it can take some people 10
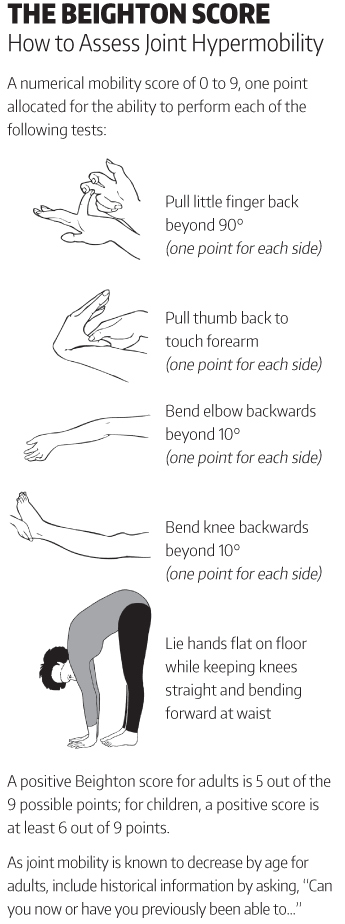
years to get a diagnosis! When my stomach pains started to get worse to the point where it hurt to eat (at the age 14), I saw a paediatric consultant at my local hospital who had coincidently just been to a medical conference linking hypermobility to stomach pain. He noticed that I was hypermobile (ie. some of my joints are extremely bendy!) and referred me to a specialist in London (Royal London Hospital) to talk more about having EDS. After that, we saw a rheumatologist who confirmed and gave me my official diagnosis. This was done by the Beighton Score and by using my medical history.
What was stoma surgery like? What happened in the hospital after surgery?
On the day of my surgery, there was actually a lot of waiting due to complications in the surgery before mine. But I had everything explained to me and was given a form to sign to say that I understood any potential risks (every surgery has some level of risk). I was given a hospital gown and some lovely compression socks (to prevent blood clots) and eventually was taken down to have my surgery. I saw the surgeon right before they put me under general anaesthetic so I could ask any last minute questions before they started. They then counted down from 10 and I think by the time they got to around 5, I was out.
I woke up a few hours later in the recovery room, very disorientated of course, and surrounded by various nurses asking if I was okay, checking on me and my newly formed stoma. My stoma was absolutely huge but that’s only because there was a lot of swelling (totally normal – it shrinks over the next few weeks!). I was wheeled in to a ward and given plenty of pain medication, before leaving me to rest. The first night, I barely slept. Not because I was in pain, I just couldn’t sleep. I was half asleep before the very strange feeling of my stoma ‘farting’ jolted me awake! It was SUCH a weird feeling at first! It really shocked me but it was a good sign – a sign that my digestive system was starting to ‘wake up’ after having had the surgery. A tiny bit of blood had leaked out from the stitches but that was fine – the nurse was on hand to help clean it up. No problem there.
The next day was the most painful day of my life. I should have asked for more medication but I assumed they would just give it to me – so my biggest tip here is, if you’re in pain ask for pain medication! It also turned out that I couldn’t pee. After having had to get out of bed (very painful and I hated the nurses for making me do that), I said that I needed the toilet but I still couldn’t physically walk to the toilet. So they made me sit on a commode (I think that’s what it’s called? Basically a portable toilet) but I couldn’t wee. So, now they had changed my bed sheets, I got back into bed and had a catheter inserted so I could feel some.. relief. Just over a litre of wee came out and I just remember the nurse laughing and saying “No wonder you were desperate!”. So I had this catheter in for a day and then I could wee normally again – yay!
I was also given this injection to help prevent blood clots, although this turned out to be very painful as the nurse injected it into my stomach so I would also advise against that! I saw the stoma nurse every day which was great. The first time I properly saw my stoma and all the stitches was when she took the bag off and changed it for me. After that, she taught me how to change a bag and how to use various products. Each day, we changed my bag together until she was confident that I knew what I was doing. She set up my first delivery for me and explained how it all worked.
Gradually, I began to walk a little more each day and I did keep having my Ensure drinks along with a vanilla mousse, which was very exciting as it was the closest thing I had had to food for over a year! I was in the hospital for 5 days in total (surgery on Friday, discharged on the Wednesday) and, after having seen a dietitian and having had my stoma supplies ordered, I was free to go! And so the process of ‘weaning’ began, where I had to gradually introduce solid food into my diet. This process took about 3 months as, by mid-September, I was fully off the Ensure drinks and had a solid and balanced diet.
What can I eat with my stoma?
I can pretty much eat anything. Before my surgery, I could have anything with gluten or dairy – it turns out that this was due to my colon not being able to digest the sugars in gluten and dairy (fructans and lactose). So I was on something called the FODMAP diet for a few years – it’s a very restrictive diet that limits the types of sugars you eat to see how your body reacts. A lot of people with IBS use this diet as well but always consult your doctor before starting any restrictive diet.
However, now with my colon ‘out of the picture’, it turns out that my stomach and small intestine are happy to digest gluten and dairy, as well as pretty much anything else (hellooo bread and cheese!). One thing that I DO have to be careful of though, is chewing. I need to make sure I chew very well, particularly fibrous foods (vegetables/fruits/nuts etc) otherwise I could get a blockage in my stoma; when output gets stuck in my small intestine, which can be very dangerous and can sometimes end up with a trip to hospital. So.. chew, chew, chew!
The only things I haven’t tried yet with my stoma as I have heard that they can cause blockages is popcorn and sweetcorn. Also, something to keep in mind, certain foods/drinks and loosen your output (fizzy drinks, alcohol, chocolate) and others can thicken it (bread, rice, pasta, bananas, peanut butter).
How often do I empty my bag and how often do I change my bag?
Depending on what I eat and drink depends on how much I empty the bag. Sometimes I can go hours and hours without emptying and sometimes I can empty it a lot in one day! Just depends what I’m doing, eating and drinking really. On average, it’s about 4-6 times a day – I usually just do it when I need to go for a wee anyway! With changing my bag, that varies too. I can go between 2 and 5 days without the need for changing it. It depends on if I have leaked (ie. if output has gone underneath the adhesive – the part of the bag that sticks to me – and onto my skin). Output is generally more acidic when you have an ileostomy, due to the acidic nature of our stomachs, and so this isn’t good for your skin which can get very sore.
What exercise can you do with a stoma?
Pretty much anything! With a stoma, you do ave to be very carful as there’s more chance of developing a hernia so you can’t jump in to do anything too strenuous. It’s a good idea to build up your core so you have more support and then you’re less likely to get a hernia or a stoma prolapse. There are also a lot of belts and support bands to help with this (Comfizz has a lot of options!) But you can run, swim, do aerobics, go hiking, do any sport – although I would recommend you get a stoma protector if you want to do contact sports. A stoma protector is basically like a plastic shield you can put on top of your stoma bag to make sure your stoma doesn’t get damaged (it can bleed very easily).
What clothes can you wear with a stoma?
Anything that is comfy! I would stay away from waistbands that go directly over your stoma, as it would get damaged that way, but apart from that, whatever you’re most comfortable with. Some people prefer low waisted, some prefer high waisted. Some stick to loose clothes, some are happy wearing tighter clothes. I can’t recommend one way in particular as everyone is different so try different styles and items of clothing and see how you (and your stoma!) feels in them.
One thing to keep in mind when, particularly when wearing tight clothes, is to make sure you don’t ‘pancake’; pancaking refers to when output gets ‘stuck’ at the top of the stoma bag, rather than go to the bottom, leading to leaks. You can prevent this by keeping your output loose or by lining the inside of you bag with a lubricant – make sure it doesn’t damage your bag though!
What products are there for stomas?
SO MANY! There are soo many options so everyone’s routine can be completely tailored and personalised for them. You have bags that come as one piece (adhesive and bag is attached) or two piece (adhesive and bag isn’t attached but you attach them together yourself). You have mini bags, midi bags and maxi bags. You have various seals, skin barriers, powders, sprays… it’s a lot to get your head around. There are many companies that offer these products AND, what’s more, they can send you free samples for you to try out! Everyone’s stoma and skin is different so taking the time figuring out what’s best for you is important.
Once you know what products you need/are best for you, you can order these online or by phone via a specialist delivery provider who will contact your GP to authorise the products being delivered and then they deliver your stoma supplies to your door. In the UK, if you have a permanent stoma, then you get these supplies for free – just talk to your GP about it and you will get a medical exemption card that means you don’t have to pay for your prescriptions.
You can change products and you can change delivery services. It’s completely flexible and up to you! If you do change delivery service, make sure you tell your GP so they know who to confirm the prescriptions to. Here’s a list of the companies and supply and/or deliver stoma supplies (note: although many of these companies are global, I only know about the ones available in the UK):
Product companies:
- Coloplast
- Salts
- Hollister (no, not the clothing brand!)
- Convatec
- Pelican Healthcare
- Dansac
- OakMed Healthcare
- CliniMed
- Trio Ostomy Care
- Peak Medical
Delivery companies (some are ‘related’ to the above companies):
- Charter (connected with Coloplast)
- Respond (connected with Pelican Healthcare)
- SecuriCare Medical (connected with CliniMed)
- Medilink (connected with Salts)
- Amcare Group (connected with Convatec)
- Fittleworth
- Bullen Healthcare
How does EDS affect my daily life?
It can definitely make me more tired. I have to pace what I’m doing so I don’t overdo it and be exhausted otherwise – easier said than done though! I also need to keep up my physio exercises to help my joints and strengthen my muscles. My joints often click, pop and partially dislocate so I do need to be careful and make sure I look after my body so that it’s strong enough.
How has my stoma and EDS affected my mental health?
In so many ways. It was particularly bad when I was a teenager, where I developed depression, anxiety and anorexia nervosa as a result of my EDS – I was embarrassed, didn’t want to tell anyone that I was basically chronically constipated and it really took a toll on my relationship with food. Since having my stoma, my relationship with food has greatly improved – I guess not eating for a whole year really makes you miss it and appreciate it once you can eat again!! I still struggle with depression and anxiety but I do know how to deal with these conditions more and definitely in a much better mental state than I was a few years ago (talking is super important, I can’t stress that enough). My stoma helped me embrace my body for the way it is and, in turn, improved my confidence a lot.

